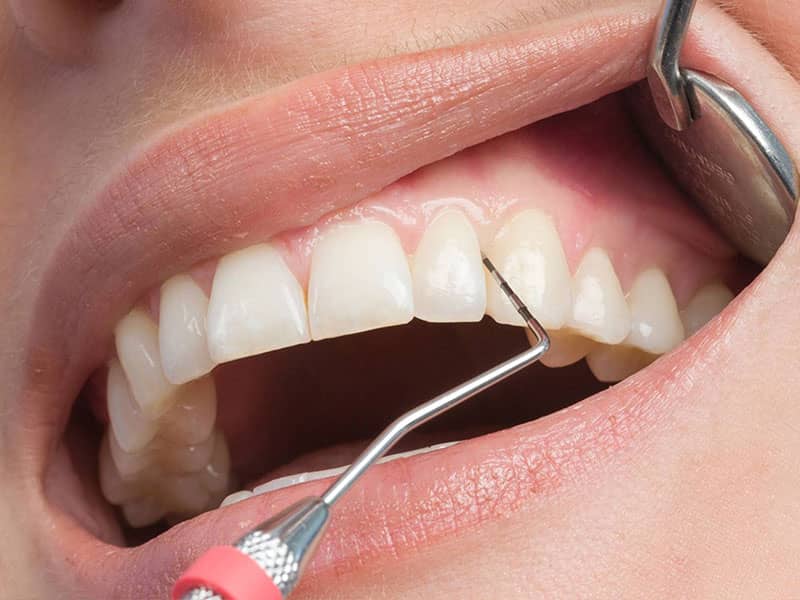
Periodontology is a branch of dentistry that deals with diseases affecting the supporting tissues of the teeth (gums and alveolar bone). The conditions treated in periodontology are typically gingivitis and periodontitis. Gingivitis is a reversible condition that occurs in the gums. However, if left untreated, it can progress to periodontitis. Also known as pyorrhea or periodontal disease, periodontitis is an inflammatory condition that affects the deeper periodontal tissues (cementum, periodontal ligament, and alveolar bone). Warning signs may include:
If not diagnosed and treated in time, periodontitis can lead to tooth loss. Periodontal diseases are mainly caused by poor oral hygiene, smoking, diabetes, and genetic predisposition. The accumulation of bacteria in the form of plaque between the teeth and gums can turn into tartar if not properly cleaned. This leads to periodontal pocket formation, tooth mobility, and destruction of periodontal tissues, ultimately resulting in tooth loss.
Individuals with poor oral hygiene and a personal predisposition are more likely to develop periodontal disease. The main causes and contributing factors include:
Depending on the stage and severity of the disease, treatment may involve anti-infective therapy, antibiotics, or surgical intervention. The progress of treatment is monitored through evaluation of clinical findings. Supportive therapy may be applied regularly to ensure long-term success. Dental cleaning is an essential part of treatment. In general, periodontal treatment includes the following steps:
A proper diagnosis based on medical history and clinical findings is essential before starting treatment. Based on the diagnosis, the dentist determines whether treatment is necessary.
During the consultation, patients are informed about their condition and diagnosis. Treatment steps and possible alternatives are discussed, including the importance of reducing risk factors such as smoking. Patients are also informed about interactions with other health conditions.
Tooth-preserving measures may be carried out before or during periodontal treatment, depending on the indication.
Patients receive specific oral hygiene instructions alongside anti-infective therapy. Gum inflammation is assessed, and patients are educated on proper oral care techniques and tools.
This is a non-surgical procedure in which all accessible soft and hard deposits, biofilm, and tartar (including subgingival tartar) are removed from periodontal pockets.
In severe cases, systemic antibiotics may be prescribed alongside anti-infective treatment.
A few months after treatment, periodontal conditions are re-evaluated. Based on the findings, further treatment is planned, and any remaining issues are addressed. Surgical treatment may be considered if necessary; otherwise, supportive therapy follows.
In some cases, surgical intervention may be required for periodontal pockets. The decision is made jointly by the dentist and the patient.
The two most important ways to prevent periodontal diseases such as gingivitis and periodontitis are:
Maintaining good oral hygiene and regularly consulting a dentist are essential for preventing dental problems. Preventive care should begin at an early age. Recent studies show that gingivitis affects 24% of individuals aged 18–30 and 27% of those aged 60–77, highlighting the importance of oral hygiene at all ages.
Teeth should be brushed using a small, soft-bristled toothbrush that is replaced frequently, along with fluoride toothpaste for added protection. Flossing is also important to clean tight spaces between teeth. Chewing increases saliva production, which helps neutralize acids produced by bacteria. Therefore, sugar-free gum can be chewed after meals.
Additionally, diet plays a crucial role. Bacteria thrive on sugar, producing acids that lead to tooth demineralization and cavities. For this reason, sugary foods should be limited.